Let me be honest with you About Diverticulitis Diet
When people hear diverticulitis, their first reaction is usually fear… followed closely by confusion about food. “Can I eat this?” “Is that going to hurt?” “Do I have to give up everything I love?”
I’ve been there—helping readers, clients, even a close friend who once looked at a bowl of popcorn like it was a ticking time bomb.
Here’s the deal.
The diverticulitis diet isn’t about punishment. It’s about timing, texture, and knowing your gut better than your favorite playlist. And yes, the science has changed. Big time.
There was a time when doctors said: avoid nuts, seeds, popcorn. Basically, anything fun. Now? Research shows those foods aren’t the villains we once thought.
So what actually works?
That’s what we’re going to unpack—slowly, clearly, and without making your head spin.
Quick Disclaimer: This article is for educational purposes only and is not a substitute for professional medical advice.
Understanding the Diverticulitis Diet: What’s Really Going On Inside Your Gut
Let’s simplify this.
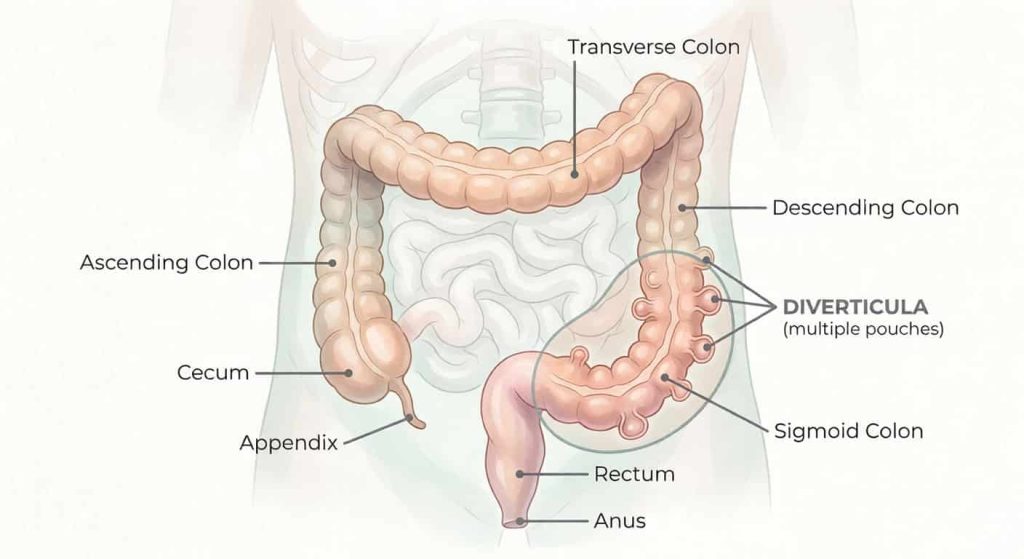
Your colon has small pouches. They’re called diverticula. Most of the time, they just sit there quietly, doing nothing dramatic.
But when they get inflamed or infected?
That’s diverticulitis. And that’s when your body starts sending loud signals—pain, bloating, fever, digestive chaos.
Now here’s where diet steps in.
Why Food Matters More Than You Think
Ever noticed how your gut reacts differently depending on what you eat?
That’s not random.
When your digestive system is irritated, it becomes sensitive. Think of it like a scraped knee—you wouldn’t rub sand on it, right?
Same idea.
During a flare-up, your gut needs rest. Gentle food. Easy digestion.
Later? It needs strength-building foods.
That’s why the diet for diverticulitis isn’t one fixed plan. It changes depending on what your body is going through.
The Two Phases of a Diverticulitis Diet
Most people don’t realize this part. And honestly, it’s where things often go wrong.
1. The Acute Phase (Flare-Up Time)
This is when symptoms are loud and clear.
Pain. Cramping. Maybe even nausea.
At this stage, your goal is simple:
👉 Give your gut a break.
We’re talking about a diverticulitis clear liquid diet or something very close to it.
We’ll go deeper into that soon.
2. The Recovery + Prevention Phase Diverticulitis Diet
Once symptoms calm down, your body shifts gears.
Now it needs:
- Fibre (yes, eventually!)
- Nutrients
- Balance
This is where a long-term diet diverticular disease approach comes into play.
And trust me—this is where most of the magic happens.
Old Myths vs New Science
Let’s clear this up quickly.
❌ Old Advice:
- No seeds
- No nuts
- No popcorn
✅ What we know now:
- These foods don’t increase risk
- Fibre actually helps prevent flare-ups
- Gut health is more about overall diet, not single foods
Crazy, right?
So if you’ve been avoiding strawberries because of the seeds… you can relax a bit.
What Your Gut Really Needs
Instead of obsessing over restrictions, think in terms of support.
Your digestive system thrives when it gets:
- Hydration (often underestimated)
- Gradual fibre increase
- Low irritation foods during recovery
- Consistency over perfection
Simple. Not always easy—but simple.
The Diverticulitis Clear Liquid Diet: Your First Step to Healing
Alright. Let’s talk about the part nobody loves—but everyone needs to understand.
The diverticulitis clear liquid diet.
Sounds boring? It kind of is.
But it works.
Why a Liquid Diet Helps During a Flare-Up
Imagine trying to digest a heavy meal when your gut is inflamed.
Not a great idea.
Liquids reduce the workload. They pass through easily. They give your colon time to calm down.
It’s not about nutrition perfection at this stage.
It’s about rest.
What You Can Actually Consume
Let’s make this practical.
During a flare-up, a liquid diet for diverticulitis typically includes:
- Clear broths (chicken or vegetable)
- Water (yes, lots of it)
- Coconut water (natural electrolytes)
- Clear fruit juices (no pulp)
- Herbal teas
- Ice pops (without fruit chunks)
Short list. But effective.
What to Avoid (Even If You’re Hungry)
This part matters.
Even “healthy” foods can irritate your gut right now.
Avoid:
- Whole fruits (too much fibre)
- Dairy (can be heavy for some)
- Solid foods of any kind
- Alcohol (definitely not your friend here)
- Caffeine (can stimulate the gut too much)
I know. It feels restrictive.
But remember—it’s temporary.
How Long Should You Stay on a Clear Liquid Diet?
Good question.
Most people stay on it for:
👉 1 to 3 days
That’s it.
If symptoms improve, you slowly move forward. Not jump. Not rush.
Slowly.
The Transition Phase (Often Ignored, But Critical)
Here’s where people mess up.
They feel slightly better… then go straight back to heavy meals.
Bad idea.
Instead, you move into a low fibre diet for diverticular disease for a short period.
Think:
- White rice
- Mashed potatoes
- Plain pasta
- Soft eggs
- Yogurt (if tolerated)
Gentle. Soft. Easy to digest.
My Honest Take (From Experience Helping Others)
I’ve seen people try to “tough it out” and skip the liquid phase.
Almost always backfires.
On the flip side, those who respect this phase?
They recover faster. With less discomfort.
It’s not glamorous. But it’s effective.
Small Tips That Make a Big Difference
You don’t need complicated hacks. Just a few smart moves:
- Sip liquids slowly instead of gulping
- Keep meals small and frequent
- Pay attention to how your body responds
- Rest. Seriously—don’t ignore this one

When to Move Forward
So how do you know you’re ready to leave the liquid phase?
Look for signs like:
- Reduced pain
- Less bloating
- Improved appetite
Your body will tell you. You just need to listen.
Building a Long-Term Diverticulitis Diet: From Fragile to Resilient Gut
So, you made it through the tough part.
The flare-up calmed down. Food doesn’t feel like the enemy anymore. That’s a win.
But now comes the real question:
👉 How do you stop this from happening again?
This is where a smart diet for diverticulitis shifts from “survival mode” to “prevention mode.”
And honestly? This phase is way more empowering.
Why Fibre Becomes Your Best Friend (Eventually)
Let’s talk fibre.
For years, people feared it during diverticular disease. Now we know better.
Fibre doesn’t hurt you. It helps you.
It keeps things moving. Reduces pressure in the colon. Prevents those little pouches from getting irritated again.
But—and this is important—you don’t jump into high fibre overnight.
You ease into it.
Types of Fibre You Should Know
Not all fibre behaves the same way.
Soluble Fibre (Gentle & Soothing)
This is your starting point.
It dissolves in water. Forms a soft gel. Easy on the gut.
Good options:
- Oats
- Bananas
- Apples (peeled at first)
- Carrots
- Sweet potatoes
Insoluble Fibre (Adds Bulk & Movement)
Helpful, but introduce slowly.
Too much too soon? That can cause discomfort.
Sources include:
- Whole grains
- Raw vegetables
- Nuts and seeds
How to Safely Increase Fibre Intake
Diverticulitis Diet
Here’s how I usually guide people:
- Start low
- Add one fibre-rich food at a time
- Drink more water (this part is non-negotiable)
- Watch your body’s signals
Simple rhythm.
No rush.

Low Fibre Diet for Diverticular Disease: When You Still Need to Be Careful
Let’s not pretend everything is perfect right after a flare-up.
Sometimes your gut stays sensitive for a while.
That’s when a temporary low fibre diet for diverticular disease makes sense.
Think of it as a bridge between healing and normal eating.
Foods That Feel “Safe” During This Phase
You want soft, low-residue foods.
Here’s what usually works well:
- White bread or toast
- White rice
- Plain pasta
- Eggs
- Lean chicken or fish
- Cooked vegetables (well-softened)
Nothing fancy. But very effective.
Foods to Limit (For Now)
Even healthy foods can wait a bit.
Try to reduce:
- Raw veggies
- Tough meats
- Whole grains (temporarily)
- Spicy or fried foods
This isn’t forever. Just until your gut stabilizes.
A Quick Reality Check
People often ask me:
“Should I stay low fibre forever?”
Short answer?
No.
Long-term low fibre isn’t ideal. It can actually increase your risk of future flare-ups.
So use it as a tool, not a lifestyle.
The Real-Life Diverticulitis Diet Plan (That You Can Actually Follow)
Let’s make this practical.
Because theory is nice—but real life is messy.
Sample Day During Recovery
Breakfast
- Soft oatmeal with banana
- Herbal tea
Lunch
- White rice with boiled chicken
- Cooked carrots
Snack
- Yogurt (if tolerated)
Dinner
- Mashed potatoes
- Steamed fish
Gentle. Balanced. No drama.
Sample Day for Long-Term Prevention
Breakfast
- Oats with berries and chia seeds
Lunch
- Quinoa salad with vegetables
Snack
- Apple with peanut butter
Dinner
- Grilled chicken
- Brown rice
- Steamed broccoli
Now you’re building resilience.
Hydration: The Quiet Hero
Let me say this clearly.
Fibre without water? Bad idea.
Water helps fibre do its job. Without it, things can get… uncomfortable.
Aim for:
- 7–9 glasses daily
- More if you’re increasing fibre
Foods People Fear (But Probably Shouldn’t)
Let’s revisit this, because it still confuses people.
Nuts and Seeds — Safe or Not?
Current research says:
👉 They’re safe.
In fact, they may even be protective.
So yes—you can enjoy:
- Almonds
- Walnuts
- Sunflower seeds
Just chew well. And don’t overdo it in one sitting.
Popcorn — The Old Villain
This one gets a bad reputation.
But there’s no solid evidence linking popcorn to flare-ups.
So if you love movie nights… you’re good.
Moderation still matters, though.
Trigger Foods: Why They’re Personal
Here’s something most guides won’t tell you.
There’s no universal “bad food” list.
What triggers one person might be totally fine for another.
That’s why I always suggest:
👉 Keep a simple food journal
Track:
- What you eat
- How you feel afterward
Patterns show up quickly.
Common Personal Triggers (But Not Guaranteed)
Some people report issues with:
- Spicy food
- Red meat
- Dairy
- Alcohol
But again—it’s personal.
Lifestyle Habits That Support Your Diverticulitis Diet
Food is only part of the story.
Your gut responds to how you live, too.
Move Your Body (Gently but Regularly)
Exercise improves digestion.
Nothing extreme needed.
- Walking
- Light stretching
- Yoga
Consistency beats intensity.
Stress: The Hidden Trigger
Ever noticed gut issues during stressful times?
That’s not in your head.
Stress affects digestion directly.
Try:
- Deep breathing
- Short breaks
- Better sleep habits
Small changes help more than you’d expect.
Read : Powerful Carnivore Diet Recipes
FAQs About the Diverticulitis Diet
Can I drink coffee?
In moderation, yes. But during flare-ups, it’s better to avoid it.
Is dairy allowed?
Depends on your tolerance. Some people handle yogurt well, others don’t.
How fast should I increase fibre?
Slowly. Over weeks, not days.
Do I need supplements?
Sometimes fibre supplements help—but food should come first.
Final Thoughts: Living Comfortably With a Diverticulitis Diet
Let me wrap this up honestly.
The diverticulitis diet isn’t about fear. It’s about awareness.
You don’t need to eat perfectly. You just need to eat intentionally.
Some days will be smooth. Others? Not so much.
That’s normal.
What matters is:
- Listening to your body
- Adjusting when needed
- Not overreacting to every symptom
Long story short—you’re in control more than you think.
And once you understand your gut?
Life starts to feel normal again.
Download your diverticulitis_diet_plan
